|
The major determinant in this intraoperative assessment process clearly relates to be the number of SLNs harvested. Defining the concept of an adequate intraoperative assessment of the axilla should be based upon any given principle that minimizes the risk of potentially failing to recognize a positive SLN and thereby assures accurate axillary staging during breast cancer surgery. Despite widespread use of this technology, very little emphasis appears to be placed on defining the adequacy of intraoperative assessment of the axilla during breast cancer surgery. The application of sentinel lymph node (SLN) mapping and biopsy to the surgical staging of the axilla during breast cancer surgery has become a universally accepted standard of practice. The scenario in which only a single negative SLN candidate is intraoperatively identified is one that should raise some concern to the operating surgeon. The accurate and optimal assessment of the axilla during breast cancer surgery requires persistence and diligence for attempting to identify all potential SLN candidates in order to avoid failing to recognize a positive SLN. A positive SLN was found in 18% (19/104) of cases when a single SLN was identified, as compared to in 34% (85/249) when two or more SLNs were identified (P = 0.003). SLN #3, SLN #4, and SLN #5 were the first positive SLN in one case (1%) each. SLN #2 was the first positive SLN in 15 (14%). SLN #1 was the first positive SLN in 86 (83%). A positive SLN was found in 104 (29%) cases. Mean number of SLNs identified was 2.5 (range, 1 to 9), with a single SLN identified in 104 (29%) cases, two identified in 110 (31%), three identified in 73 (21%), four identified in 35 (10%), five identified in 16 (5%), and six or more identified in 15 (4%). ResultsĪmong 371 invasive breast cancers, a SLN was identified within 353 cases (95%). All potential SLN candidates, containing counts of at least 10% of the hottest SLN and/or containing blue dye, were harvested and were consecutively numbered in the order of the decreasing level of counts (with the hottest SLN representing SLN #1). A combined radiocolloid and blue dye technique was used. We retrospectively analyzed a series of 400 breast cancers from a recently published prospective randomized clinical trial. The aim of the current study was to assess when metastatic disease was first identified within consecutively harvested SLN candidates for invasive breast cancers demonstrating a positive SLN. 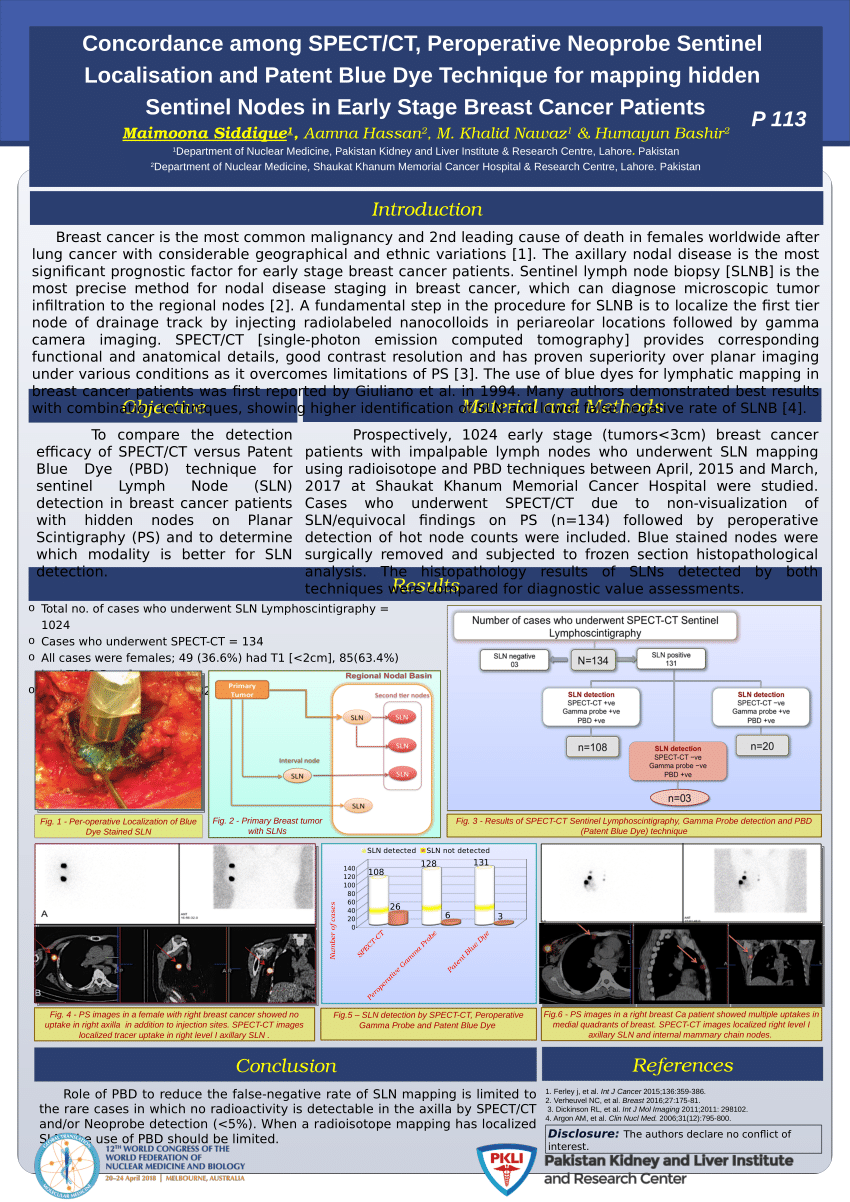 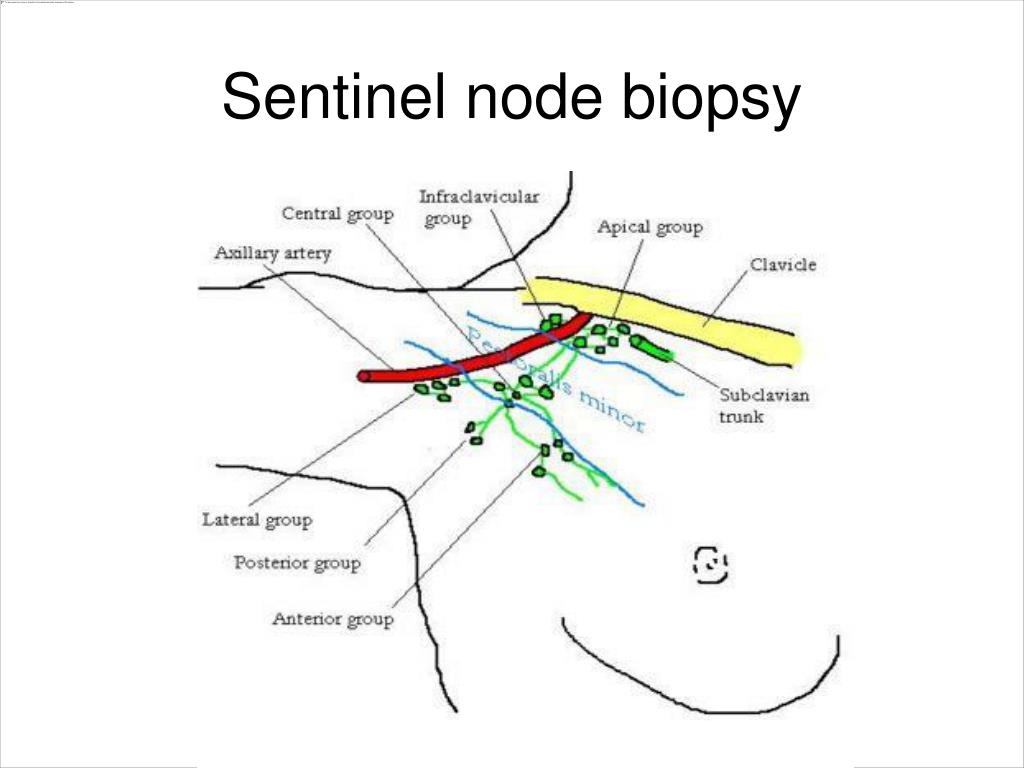
Although sentinel lymph node (SLN) biopsy is a standard of care for the evaluation of the axillary lymph nodes during breast cancer surgery, a substantial degree of variation exists among individual surgeons as to what represents an adequate assessment.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
